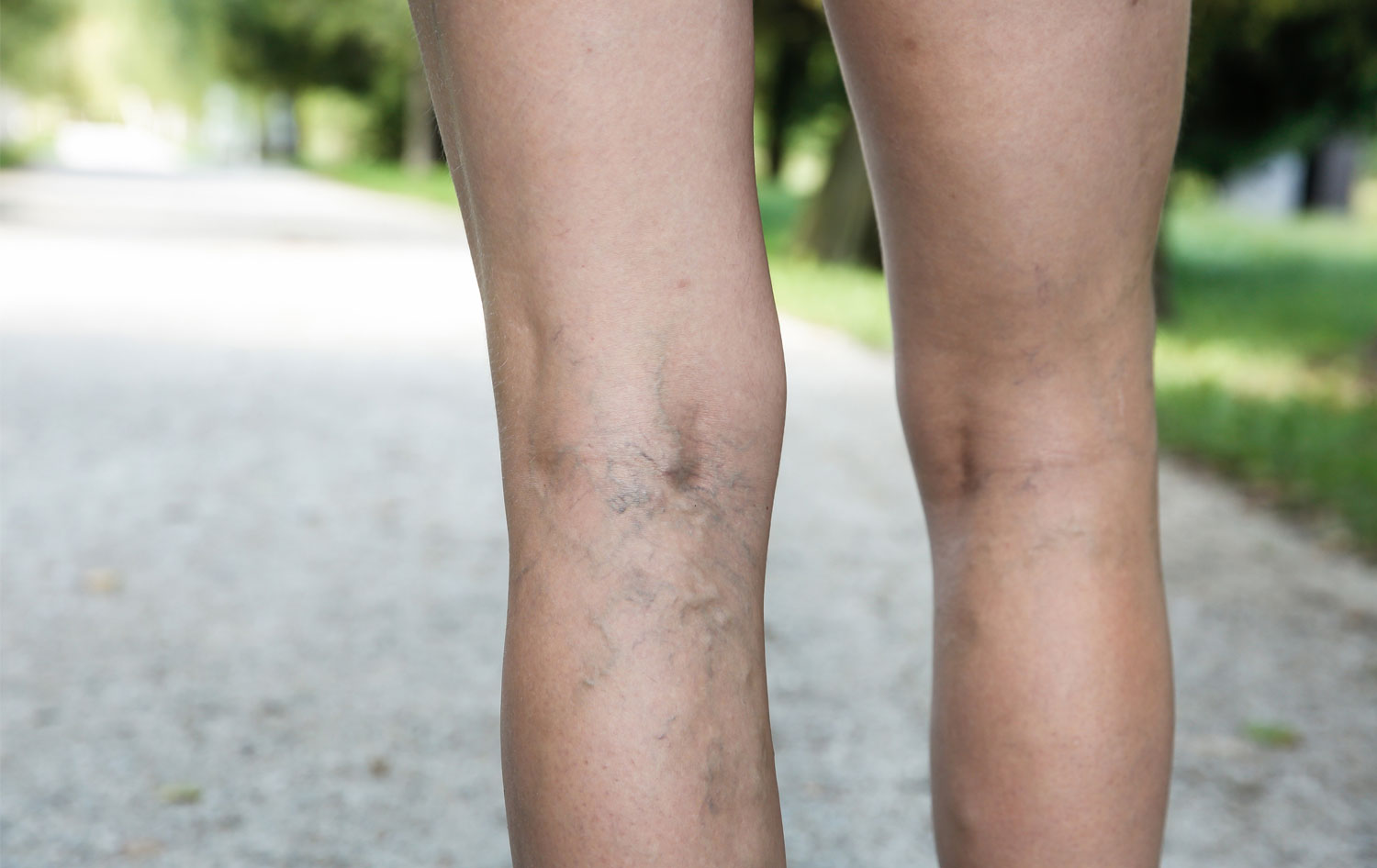
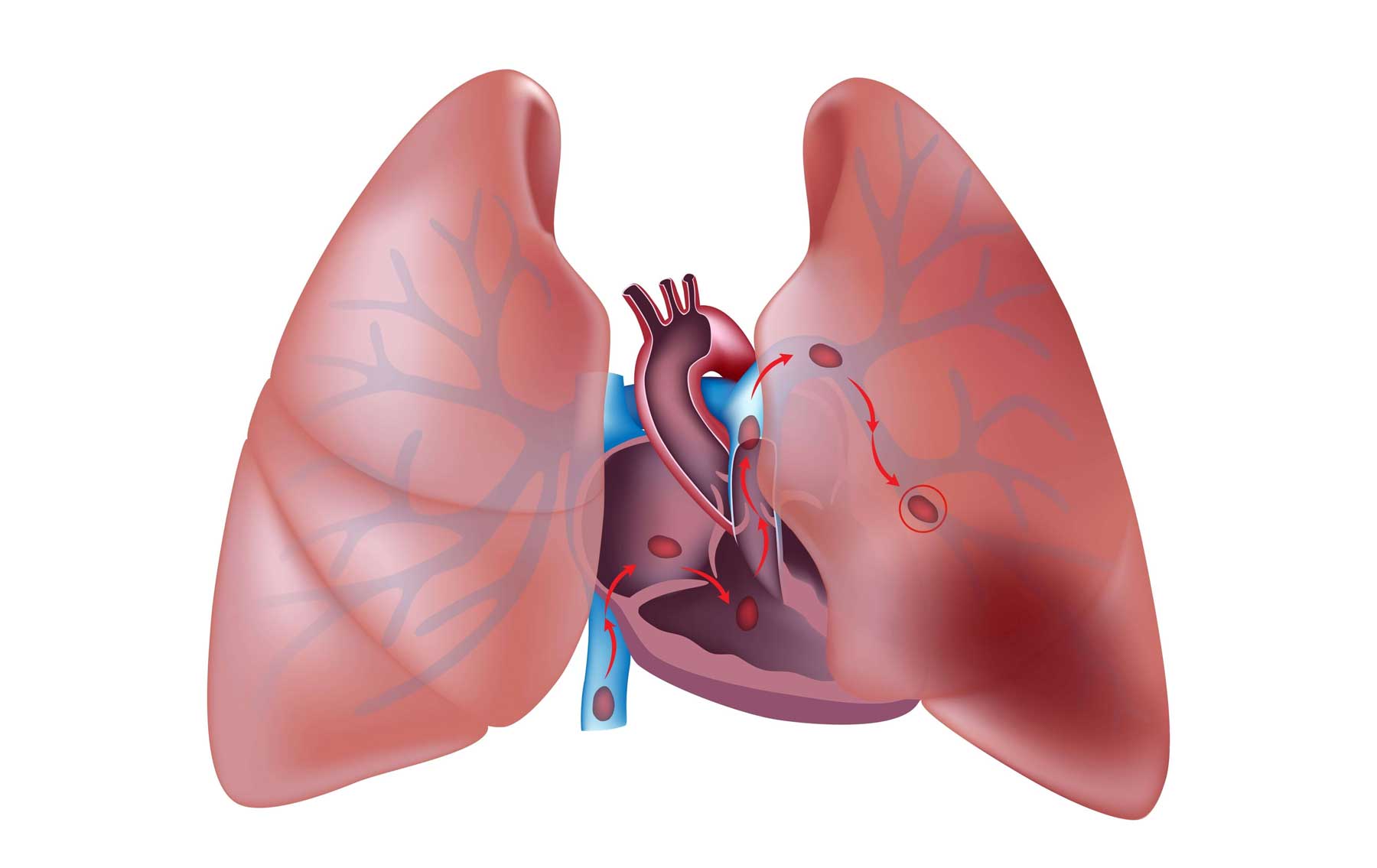
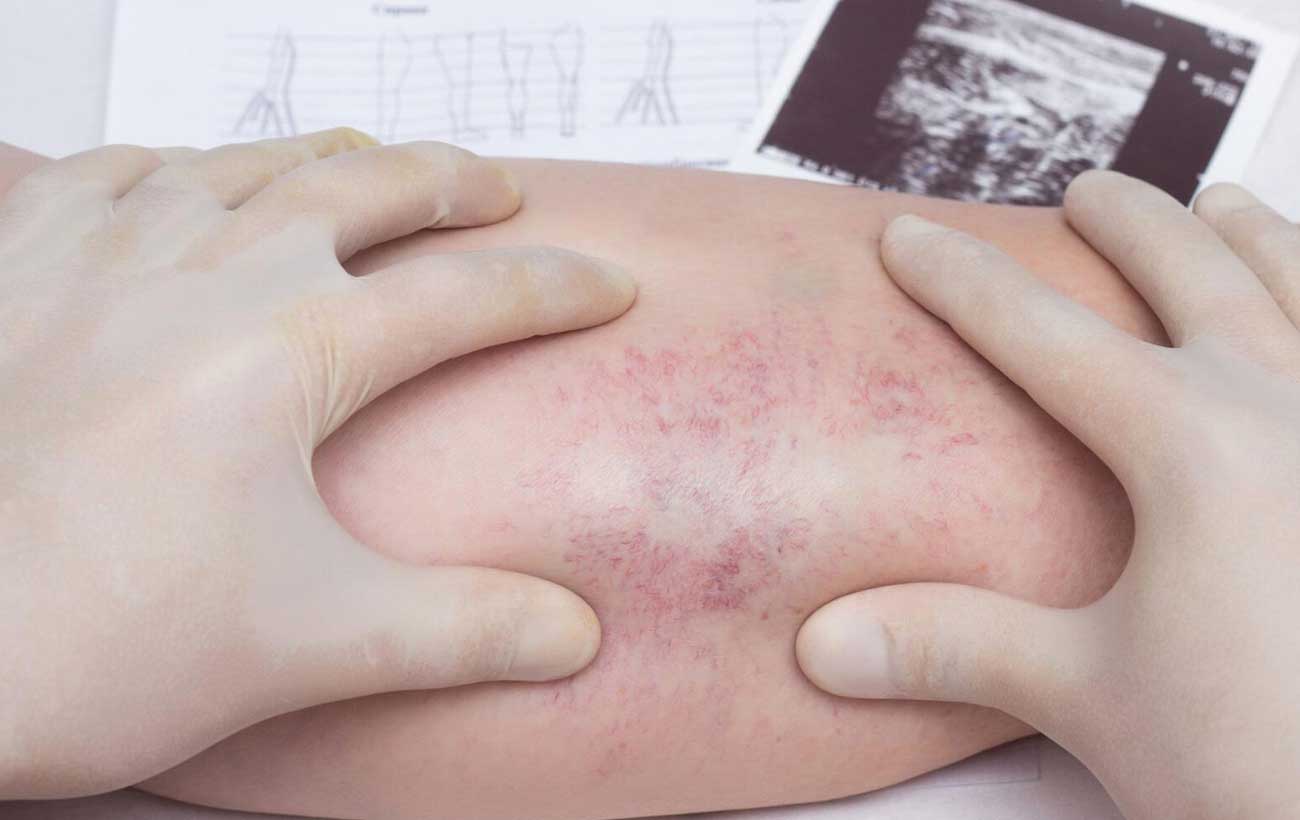
Deep Vein Thrombosis Thrombosis is the formation of a blood clot (thrombus), which can partially…
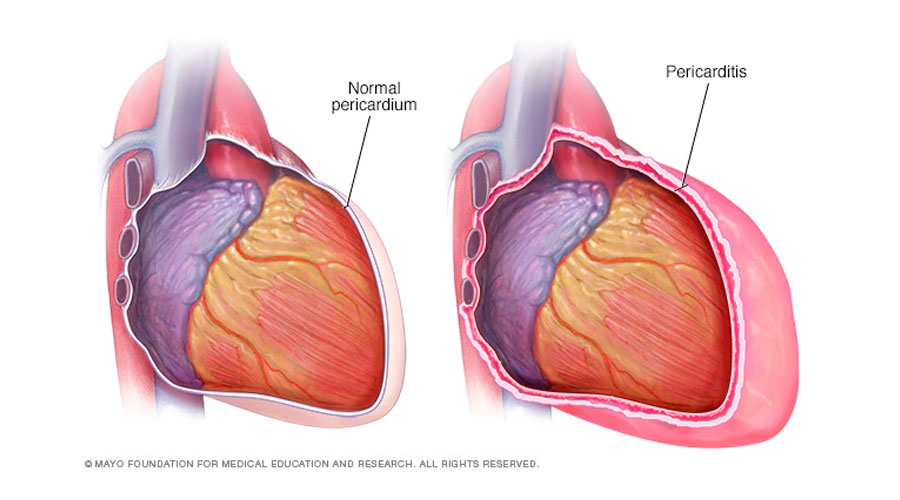
Acute Pericarditis
Pericarditis is inflammation of the pericardium, the membrane that surrounds the heart. When the pericardium becomes inflamed, fluid can collect in the space between the membrane and the heart (called pericardial effusion). The inflammation in acute pericarditis is usually caused by a viral infection, but it can also result from tuberculosis, rheumatic fever, a disease of connective tissue such as lupus, or chronic kidney failure. In rare cases, acute pericarditis follows a heart attack or a chest injury. Pericarditis often occurs along with more serious illness and occasionally can follow open-heart surgery.
Symptoms
The main symptom of acute pericarditis is severe pain, usually in the center of the chest, that may radiate to the left shoulder. The pain of acute pericarditis becomes worse if you breathe deeply, cough, or twist your body. Chest pain, especially if it occurs along with breathing difficulty, can be a symptom of a serious illness such as pneumonia, pulmonary embolism, and heart attack.
You may also be short of breath and have a slight fever. As fluid collects around the heart, it creates pressure that can interfere with the normal filling of the heart with blood and cause a severe decrease in the volume of blood pumped by the heart, which can lead to death.
Treatments
Acute pericarditis caused by a viral infection usually clears up without treatment. If the pain is severe, the doctor will probably prescribe a nonsteroidal anti-inflammatory drug such as aspirin, ibuprofen, or indomethacin. The doctor may insert a needle into the chest to remove some of the fluid and relieve pressure on the heart.
The inflammation usually subsides within 10 to 14 days and leaves no aftereffects. In rare cases, such as when acute pericarditis occurs a few weeks after a heart attack, a doctor may prescribe a corticosteroid drug to reduce inflammation. When acute pericarditis results from a connective tissue disorder or a metabolic disorder, the underlying disease must be treated.