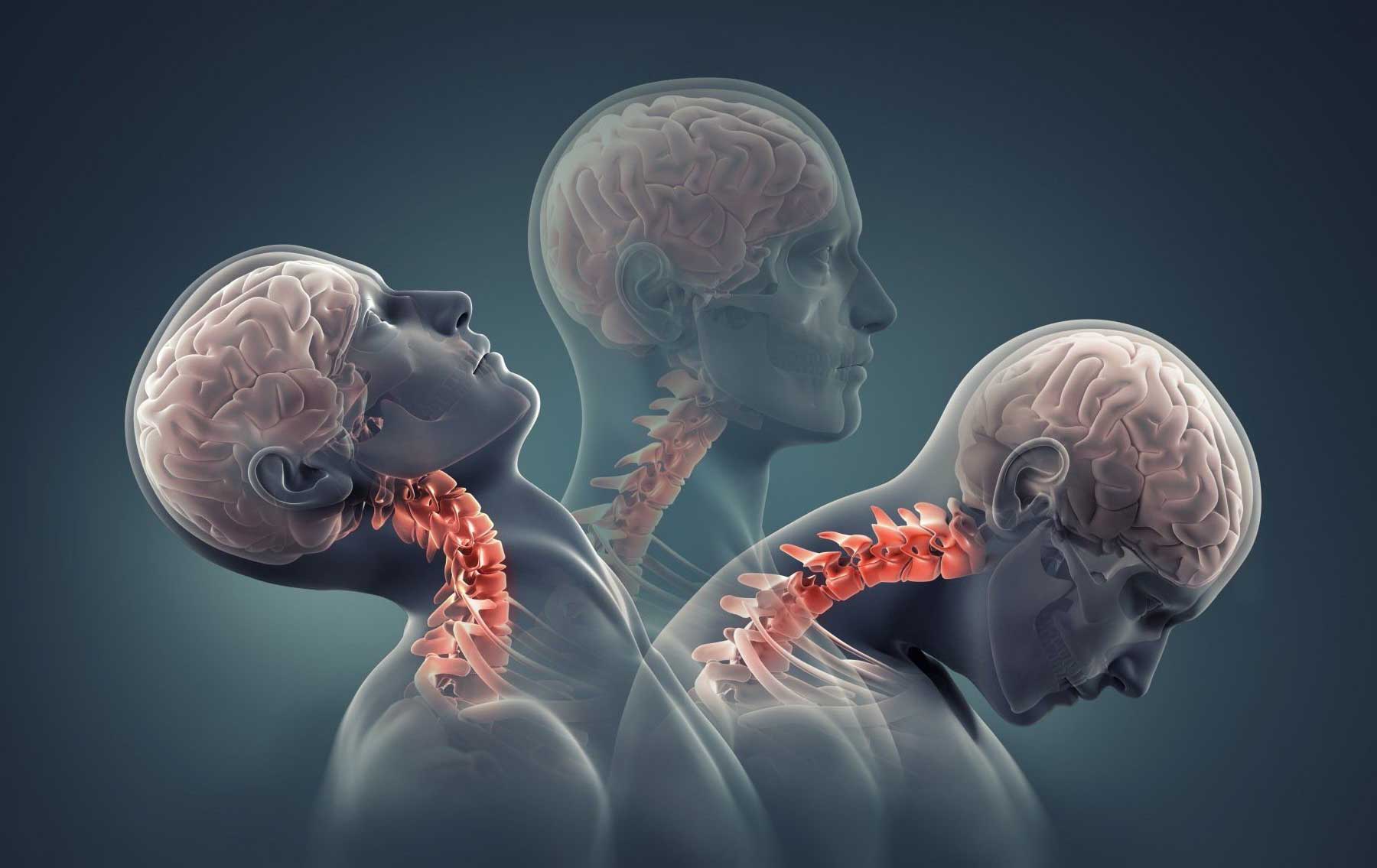
Traumatic Brain Injury
A traumatic brain injury (TBI) is defined as a blow to the head or a penetrating head injury that disrupts the normal function of the brain. TBI can result when the head suddenly and violently hits an object or when an object pierces the skull and enters brain tissue. Symptoms of a TBI can be mild, moderate or severe, depending on the extent of damage to the brain. Mild cases may result in a brief change in mental state or consciousness, while severe cases may result in extended periods of unconsciousness, coma or even death.
Treatments
Surgical Treatment
Many patients with moderate or severe head injuries are taken directly from the emergency room to the operating room. In many cases, surgery is performed to remove a large hematoma or contusion that is significantly compressing the brain or raising the pressure within the skull. After surgery, these patients are usually observed and monitored in the intensive care unit (ICU).
Other head-injured patients may not go to the operating room immediately, but instead are taken from the emergency room to the ICU. Contusions or hematomas may enlarge over the first hours or days after head injury, so some patients are not taken to surgery until several days after an injury. Delayed hematomas may be discovered when a patient’s neurological exam worsens or when their ICP increases. On other occasions, a routine follow-up CT scan that was ordered to determine if a small lesion has changed in size indicates that the hematoma or contusion has enlarged significantly. In many cases, removing the lesion before it enlarges and causes neurological damage may be the safest approach for the patient.
At surgery, the hair over the affected part of the head is usually shaved. After the scalp incision is made, the bone that is removed is usually taken out in a single piece or flap, which is then replaced after surgery. Sometimes, however, the bone may be shattered or heavily contaminated. In these cases, the contaminated or shattered fragments may be removed and not replaced. The dura mater is carefully cut to reveal the underlying brain. After any hematoma or contusion is removed, the neurosurgeon ensures that the area is not bleeding. He or she then closes the dura, replaces the bone and closes the scalp. If the brain is very swollen, some neurosurgeons may decide not to replace the bone until the swelling decreases, which may take up to several weeks. The neurosurgeon may elect to place an ICP monitor or other types of monitors if these were not already in place. The patient is then returned to the ICU for observation and additional care.
Medical Treatment
At the present time, there is no medication or “miracle treatment” that can be given to prevent nerve damage or promote nerve healing after TBI. The primary goal in the ICU is to prevent any secondary injury to the brain. The “primary insult” refers to the initial trauma to the brain, whereas the “secondary insult” is any subsequent development that may contribute to neurological injury. For example, an injured brain is especially sensitive and vulnerable to decreases in blood pressure that might otherwise be well tolerated. One way of avoiding secondary insults is to try to maintain normal or slightly elevated blood pressure levels. Likewise, increases in ICP, decreases in blood oxygenation, increases in body temperature, increases in blood glucose and many other disturbances can potentially worsen neurological damage. The prevention of secondary insults is a major part of the ICU management of head-injured patients.
Various monitoring devices may assist health care personnel in caring for the patient. Placement of an ICP monitor into the brain itself can help detect excessive swelling of the brain. One commonly used type of ICP monitor is a ventriculostomy, which is a narrow, flexible, hollow catheter that is passed into the ventricles, or fluid spaces in the center of the brain, to monitor ICP and to drain CSF if ICP increases. Another commonly used type of intracranial pressure monitoring device involves placement of a small fiberoptic catheter directly into the brain tissue. Additional catheters may be added that measure brain temperature and brain tissue oxygenation. Placement of an oxygen sensor into the jugular vein can detect how much oxygen in the blood is arising from the brain and can indicate how much oxygen the brain is using. This may be related to the degree of brain damage. Many other monitoring techniques are currently under investigation to see if they can help to improve outcome after head injury or provide other critical information about caring for TBI patients.