Cauda equina syndrome (CES)
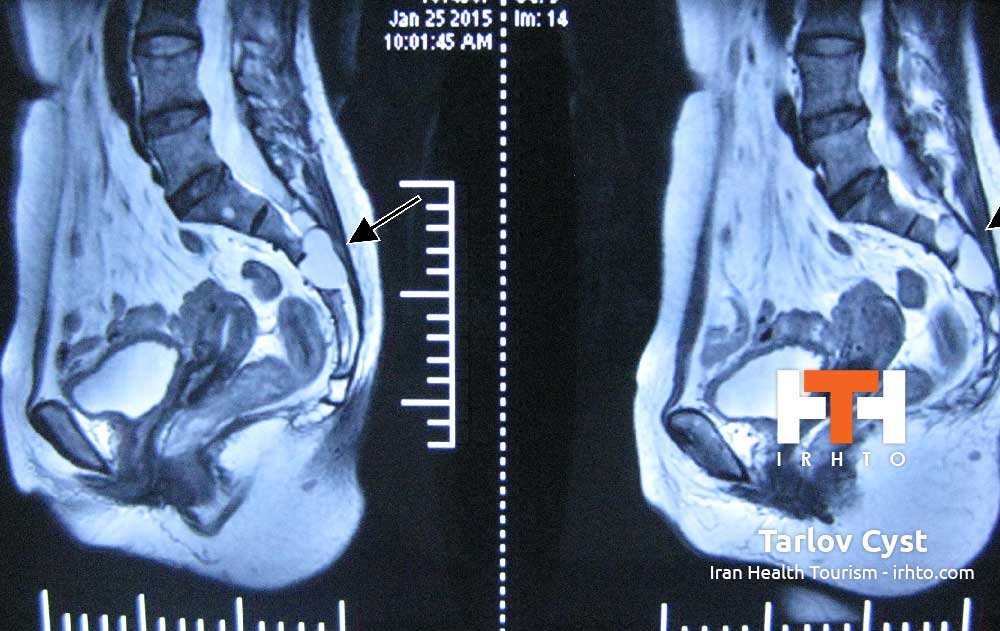
Low back pain affects millions of people every year and, in most cases, it improves without surgery. But severe back pain can be a symptom of a serious condition that is not well known and is often misdiagnosed. Cauda equina syndrome (CES) occurs when the nerve roots of the cauda equina are compressed and disrupt motor and sensory function to the lower extremities and bladder. Patients with this syndrome are often admitted to the hospital as a medical emergency. CES can lead to incontinence and even permanent paralysis.
Causes [h4]
CES most commonly results from a massive herniated disc in the lumbar region. A single excessive strain or injury may cause a herniated disc. However, disc material degenerates naturally as a person ages, and the ligaments that hold it in place begin to weaken. As this degeneration progresses, a relatively minor strain or twisting movement can cause a disc to rupture.
The following are other potential causes of CES:
- Spinal lesions and tumors
- Spinal infections or inflammation
- Lumbar spinal stenosis
- Violent injuries to the lower back (gunshots, falls, auto accidents)
- Birth abnormalities
- Spinal arteriovenous malformations (AVMs)
- Spinal hemorrhages (subarachnoid, subdural, epidural)
- Postoperative lumbar spine surgery complications
- Spinal anesthesia
Treatments [h4]
Once the diagnosis of CES is made, and the etiology established, urgent surgery is usually the treatment of choice. The goal is to reverse the symptoms of neural dysfunction. Left untreated, CES can result in permanent paralysis and incontinence.
Those experiencing any of the red flag symptoms should consult a neurosurgeon as soon as possible. Prompt surgery is the best treatment for patients with CES. Treating patients within 48 hours after the onset of the syndrome provides a significant advantage in improving sensory and motor deficits as well as urinary and rectal function. But even patients who undergo surgery after the 48-hour ideal time frame may experience considerable improvement.
Although short-term recovery of bladder function may lag behind reversal of lower extremity motor deficits, the function may continue to improve years after surgery. Following surgery, drug therapy coupled with intermittent self-catheterization can help lead to a slow but steady recovery of bladder and bowel function.